
Patient-Driven Payment Model (PDPM), Audits, and Documentation: Why the Therapist You Place Matters as Much as the Fact That You Place One
COMPLIANCE & RISK | SNF OPERATIONS
Patient-Driven Payment Model (PDPM), Audits, and Documentation: Why the Therapist You Place Matters as Much as the Fact That You Place One

When a skilled nursing facility (SNF) has an open physical therapy (PT) slot to fill, the pressure to fill it fast is real. Census is up, the schedule is stretched, patients are waiting, and the phone call to a staffing agency feels like a solution.
And it is — as long as the therapist who shows up knows what they're doing. Not just clinically, but administratively. In a SNF operating under Medicare's Patient-Driven Payment Model (PDPM), documentation errors made by a contract therapist don't just hurt the patient. They can trigger claim denials, audit findings, and in serious cases, repayment demands from the Centers for Medicare & Medicaid Services (CMS).
This is the part of contract staffing that most agencies don't talk about. We will.
The Compliance Landscape Has Gotten Harder
PDPM, which replaced the old Resource Utilization Group (RUG) IV payment system on October 1, 2019, fundamentally changed how SNF reimbursement works. Under the previous system, therapy volume was a primary driver of payment. Under PDPM, reimbursement is driven by patient characteristics — diagnosis, functional status, comorbidities — and the documentation that captures those characteristics.
That shift placed enormous weight on the accuracy and specificity of clinical documentation. And the data shows that many facilities haven't fully adapted.
17.2%
Improper payment rate for SNF Medicare services in 2024
— approximately $5.9 billion in projected improper payments | CMS CERT Program, 2024
That number — 17.2% — represents a dramatic increase from 7.79% in 2021. CMS took notice. The agency launched the SNF 5-Claim Probe and Educate Review in June 2023, which subjected every Medicare-billing SNF in the country to a claim review. And the most common reason for denials? Not fraud. Not billing errors. Documentation deficiencies.
In fact, according to CMS Supplemental Improper Payment Data, insufficient documentation accounted for nearly 79.1% of improper payments in SNF Part A claims. That is a documentation problem — and documentation is written by therapists.
In 2026, the scrutiny has intensified further. The HHS Office of Inspector General (OIG) has initiated a new audit series specifically examining SNF use of PDPM. CMS's FY 2026 SNF billing rule expanded audit scope to include PDPM upcoding, lack of medical necessity, improper therapy billing, and billing errors under SNF Consolidated Billing — and auditors are actively comparing Minimum Data Set (MDS) submissions against supporting clinical documentation to find discrepancies.
What Poor Therapy Documentation Actually Triggers
It's worth being specific about what goes wrong — because the risks aren't abstract.
MDS and Documentation Misalignment
The Minimum Data Set (MDS) is the assessment tool that drives PDPM classification and payment. Functional scoring in Section GG — which captures a patient's ability to perform self-care and mobility tasks — directly affects the PT and Occupational Therapy (OT) case-mix components that determine payment rates. If a contract therapist scores Section GG inaccurately, or if their therapy notes don't support the MDS coding, CMS auditors can recode the claim and reduce reimbursement.
Medical Necessity Gaps
PDPM does not set mandatory therapy hour minimums, but it does require that every therapy visit be medically necessary and documented as such. Vague progress notes, templated language, or notes that fail to connect the therapy intervention to the patient's clinical condition are the most common trigger for denied claims and audit findings. A therapist who isn't trained in PDPM-specific documentation standards will routinely produce notes that create this exposure.
Group and Concurrent Therapy Cap Violations
Under PDPM, group and concurrent therapy are capped at 25% of total therapy minutes per discipline, per patient stay. Auditors actively review therapy logs to verify compliance with this threshold. A contract therapist unfamiliar with this rule — or who came from an outpatient setting where these limits don't apply — can inadvertently push a facility over the threshold.
KX Modifier Failures (Medicare Part B)
For Medicare Part B therapy services, the KX modifier is required when a patient exceeds the annual therapy threshold ($2,410 for PT and Speech-Language Pathology combined in 2025). This modifier is an attestation that continued therapy is medically necessary, and the rationale must be documented in the medical record. Claims submitted without the modifier — or without supporting documentation — are automatically denied.
Filling a therapy slot doesn't protect your facility from audit risk. Filling it with a clinician who understands SNF compliance does.
What a Proper Vetting Process Should Cover
Most facilities ask staffing agencies one question when requesting a contract therapist: is this person licensed? That's a necessary starting point. It is not a sufficient one.
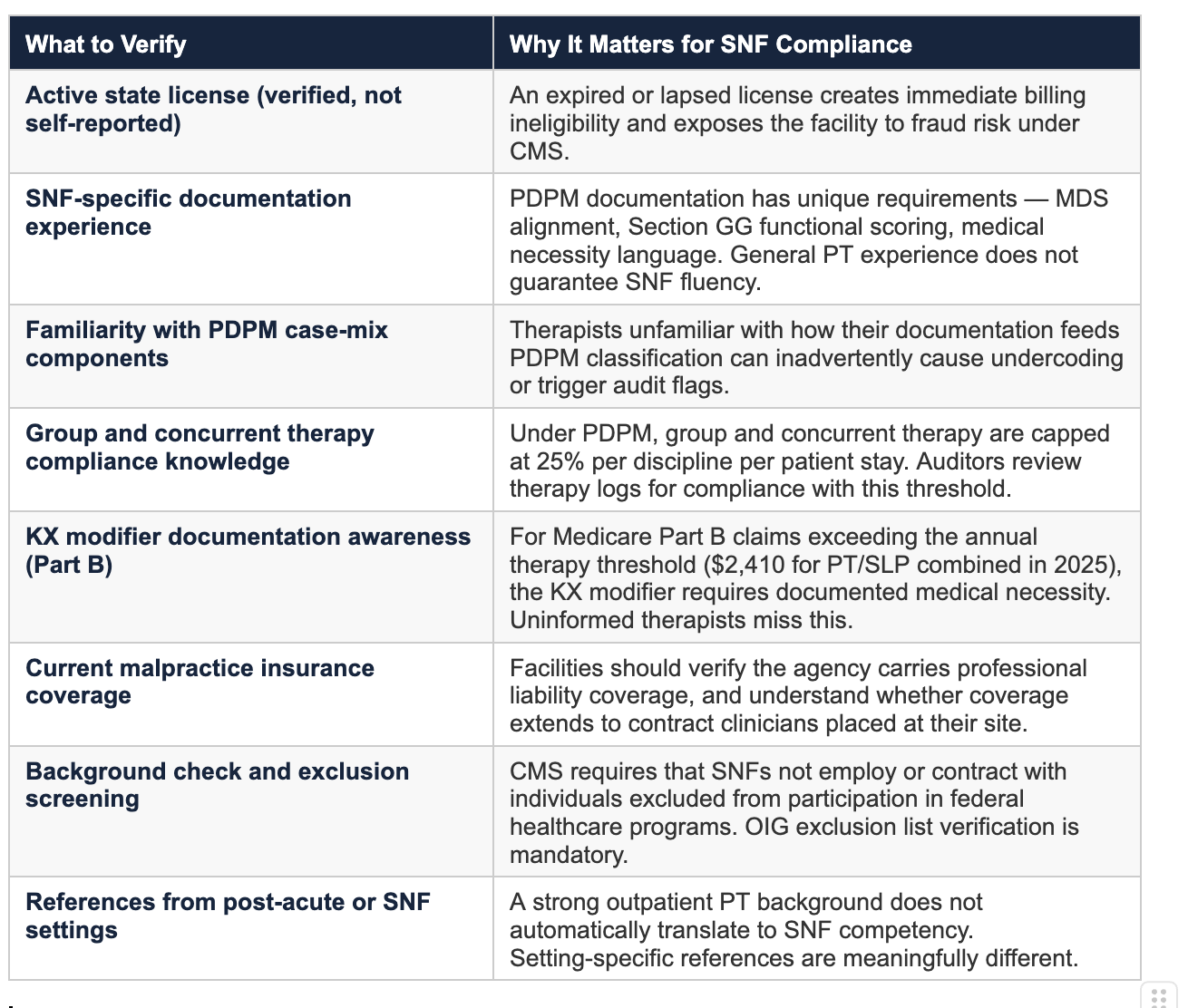
Here is what a rigorous vetting process for a contract PT or Physical Therapist Assistant (PTA) placed in a SNF should actually cover:
What to Verify
Why It Matters for SNF Compliance
Active state license (verified, not self-reported)
An expired or lapsed license creates immediate billing ineligibility and exposes the facility to fraud risk under CMS.
SNF-specific documentation experience
PDPM documentation has unique requirements — MDS alignment, Section GG functional scoring, medical necessity language. General PT experience does not guarantee SNF fluency.
Familiarity with PDPM case-mix components
Therapists unfamiliar with how their documentation feeds PDPM classification can inadvertently cause undercoding or trigger audit flags.
Group and concurrent therapy compliance knowledge
Under PDPM, group and concurrent therapy are capped at 25% per discipline per patient stay. Auditors review therapy logs for compliance with this threshold.
KX modifier documentation awareness (Part B)
For Medicare Part B claims exceeding the annual therapy threshold ($2,410 for PT/SLP combined in 2025), the KX modifier requires documented medical necessity. Uninformed therapists miss this.
Current malpractice insurance coverage
Facilities should verify the agency carries professional liability coverage, and understand whether coverage extends to contract clinicians placed at their site.
Background check and exclusion screening
CMS requires that SNFs not employ or contract with individuals excluded from participation in federal healthcare programs. OIG exclusion list verification is mandatory.
References from post-acute or SNF settings
A strong outpatient PT background does not automatically translate to SNF competency. Setting-specific references are meaningfully different.
The Setting-Specific Experience Gap Is Real
This point deserves emphasis, because it's the one most often missed in a rush to fill a slot.
Physical therapy in a skilled nursing facility is a distinct clinical and administrative environment. The patient population is older, medically complex, and often post-acute. The documentation standards are governed by Medicare Part A rules and PDPM classification requirements that simply don't exist in outpatient orthopedic or sports medicine settings. The Interdisciplinary Team (IDT) meeting structure, the MDS cycle, the care planning requirements — these are SNF-specific workflows that a therapist either knows or doesn't.
A 2025 study in Physical Therapy Journal confirmed that about 1 in 4 physical therapists works in a hospital-based setting, meaning a substantial portion of the therapist workforce has limited exposure to post-acute documentation requirements. Placing a highly skilled outpatient therapist in a SNF without verifying their post-acute experience is a compliance risk that shows up in the chart — and eventually in the audit.
What to Ask Your Staffing Agency
If you're working with a staffing agency to fill PT or PTA positions at your SNF, these are the questions worth asking before you agree to a placement:
Do you verify state licensure directly, or rely on self-reported documentation? Verification through the state licensing board or a primary source verification service is the standard. Agencies that rely on applicant-submitted documents create licensing gap risk.
How do you screen for SNF-specific documentation experience? Ask whether the agency reviews prior employment settings, references from post-acute facilities specifically, and familiarity with PDPM and MDS workflows.
Do your placements carry professional liability insurance? Understand whether the agency's coverage extends to contract clinicians placed at your facility, and what the coverage limits are.
Do you conduct OIG exclusion list screening? This is a CMS compliance requirement for SNFs — any individual excluded from federal healthcare programs cannot be employed or contracted. Confirm the agency runs this check.
Can you provide references from SNF placements specifically? Setting-specific references are meaningfully different from general professional references. A strong outpatient history tells you little about SNF documentation competency.
The Bottom Line
Contract staffing is a legitimate and often necessary tool for SNF operations. The facilities using it most effectively aren't just filling shifts — they're asking the right questions about who is filling them.
PDPM raised the stakes for clinical documentation in ways that are still catching facilities off guard years after implementation. Audit activity is increasing, not decreasing. The improper payment rate is still climbing. And the documentation that drives it is written — or not written correctly — by the therapists in your building.
Choosing a staffing partner that vets for SNF-specific compliance competency — not just licensure — is one of the most straightforward ways to reduce that exposure. The therapist you place matters as much as the fact that you placed one.
CoreEthos Group serves SNFs, home health agencies, outpatient clinics, and inpatient rehabilitation facilities (IRFs) across the DC, Maryland, and Virginia region. We vet every PT and PTA candidate for state licensure, post-acute experience, PDPM documentation familiarity, OIG exclusion status, and professional liability coverage — because placing the right clinician means more than placing a licensed one.
Have questions about how we screen our candidates? We're glad to walk you through our process.